Cytotoxic T lymphocytes act as the immune system’s specialized “killer” cells, seeking out and eliminating infected or cancerous cells with remarkable precision. Their effectiveness depends on a tightly controlled contact point called the “immune synapse,” where they release toxic molecules that destroy the target while leaving surrounding healthy cells unharmed. Until recently, scientists struggled to observe the fine structure of this process in detail. Now, researchers from the University of Geneva (UNIGE) and the Lausanne University Hospital (CHUV) have managed to visualize these mechanisms in three dimensions under near-native conditions. Their findings, published in Cell Reports, shed new light on how the internal organization of cytotoxic T cells supports their function and could advance research in immuno-oncology.
When the body faces infection or cancer, cytotoxic T lymphocytes bind tightly to their target and form the immune synapse. Through this specialized interface, they release toxic substances that trigger the destruction of the harmful cell. This targeted approach allows the immune system to remove threats efficiently while minimizing collateral damage to nearby tissue.
Although scientists have long understood the basics of this process, studying its detailed structure at the nanometer scale inside intact human cells has remained challenging. A major difficulty comes from how samples are prepared, since traditional methods can distort delicate cellular components. Existing imaging techniques often force researchers to choose between high resolution, a large field of view, or preserving the cell’s natural structure.
Cryo-Expansion Microscopy Reveals Hidden Details
To overcome these challenges, the UNIGE and CHUV-UNIL team, supported by the ISREC Foundation TANDEM program, used an advanced method called cryo-expansion microscopy (cryo-ExM). “This technique involves instantaneously freezing cells at very high speed, placing them in a so-called vitreous state, where water solidifies without forming crystals and thus faithfully preserves biological structures. The samples are then physically expanded using an absorbent hydrogel, making it possible to observe their internal organization with great precision while maintaining their near-native architecture,” explains Virginie Hamel, Senior Lecturer in the Department of Molecular and Cellular Biology at the Faculty of Science of UNIGE.
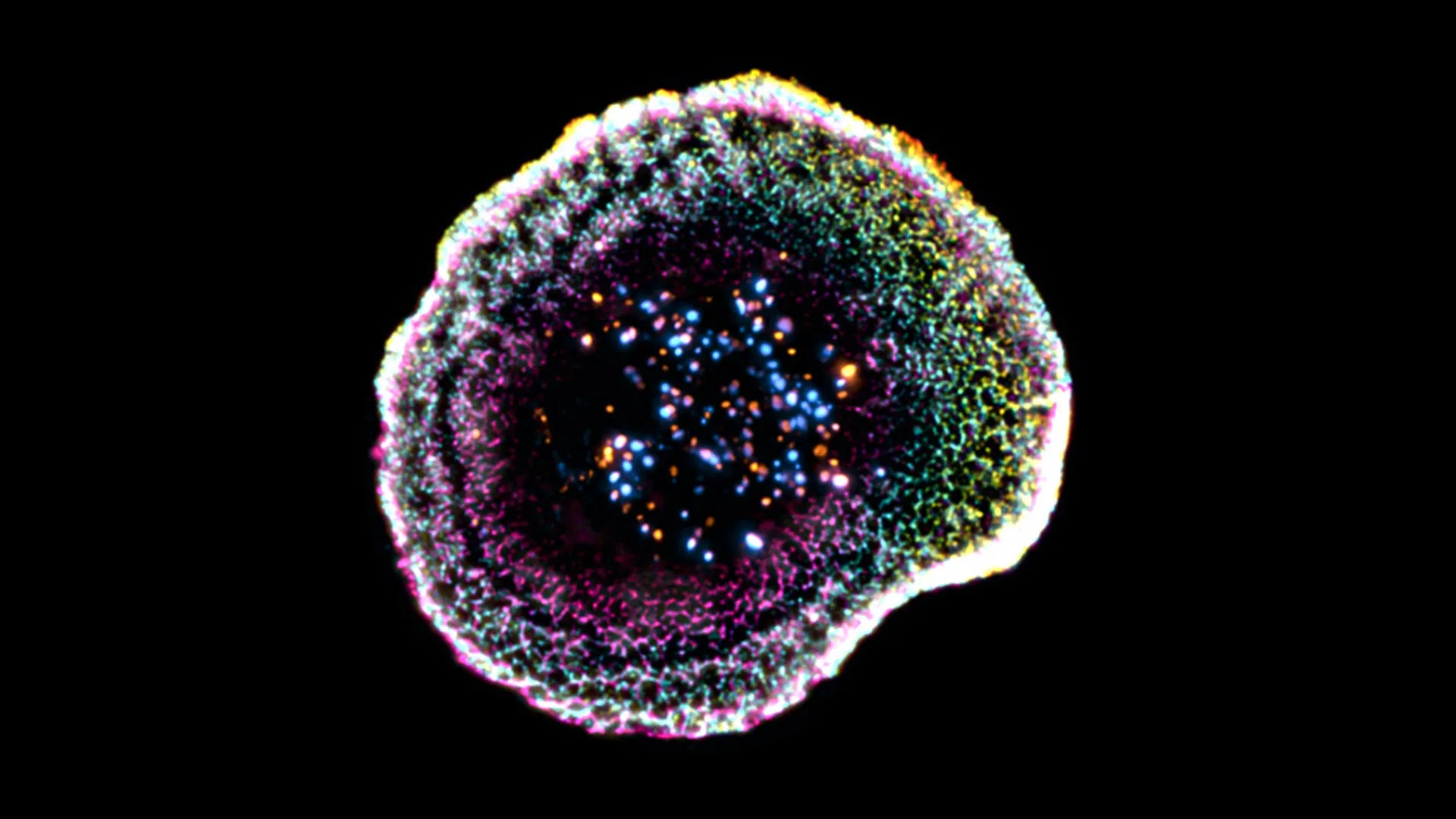
Using this approach, the researchers uncovered new structural features at the point where the immune cell meets its target. “Our work reveals that at the point of contact between the immune cell and its target, the membrane forms a kind of dome, whose structure appears to be linked to adhesion interactions and to the internal organization of the cell,” notes Florent Lemaître, postdoctoral researcher in the Department of Molecular and Cellular Biology at the Faculty of Science of UNIGE and first author of the study. The team also examined cytotoxic granules, which are responsible for killing target cells, with unprecedented clarity. They found that these granules can differ in structure, sometimes containing one or multiple “cores” where the active molecules are concentrated.
From Laboratory Cells to Real Tumors
The researchers extended their method beyond isolated cells and applied it directly to human tumor samples. “We extended this approach to human tumor tissues, making it possible to directly observe T lymphocytes infiltrating tumors and their cytotoxic machinery at the nanometer scale. This allows us to study immune responses directly in their clinical context and to better understand the mechanisms that determine their effectiveness,” explains Benita Wolf, Chief Resident and Associate Researcher in the Department of Clinical Oncology at CHUV, who co-led the study.
By providing a three-dimensional and near-native view of how these immune cells operate, the work offers a valuable framework for studying immune responses in real-world conditions. These insights could help refine treatments, especially in immuno-oncology, by improving our understanding of what drives successful immune attacks against cancer and what limits them.